Chai Shots #002: ACC Guidelines and South Asian Cardiometabolics
A New Blueprint, Some Thoughts..But Where’s the Mitochondria?
Welcome back to Chai Shots, where we distill the latest science in longevity, metabolism, and South Asian health, preferably with a cup of kadak chai.
This week, we’re diving into a landmark piece of guidance: the American Society for Preventive Cardiology (ASPC) Clinical Practice Statement focused entirely on improving cardiometabolic health for South Asians in North America. This isn’t just another medical paper; it’s a necessary, culturally tailored blueprint designed to confront the disproportionate risk we face. It’s a huge step forward to see a major cardiology body admit that the one-size-fits-all guidelines simply do not work for our unique genetic and lifestyle milieu.
What’s This Paper About?
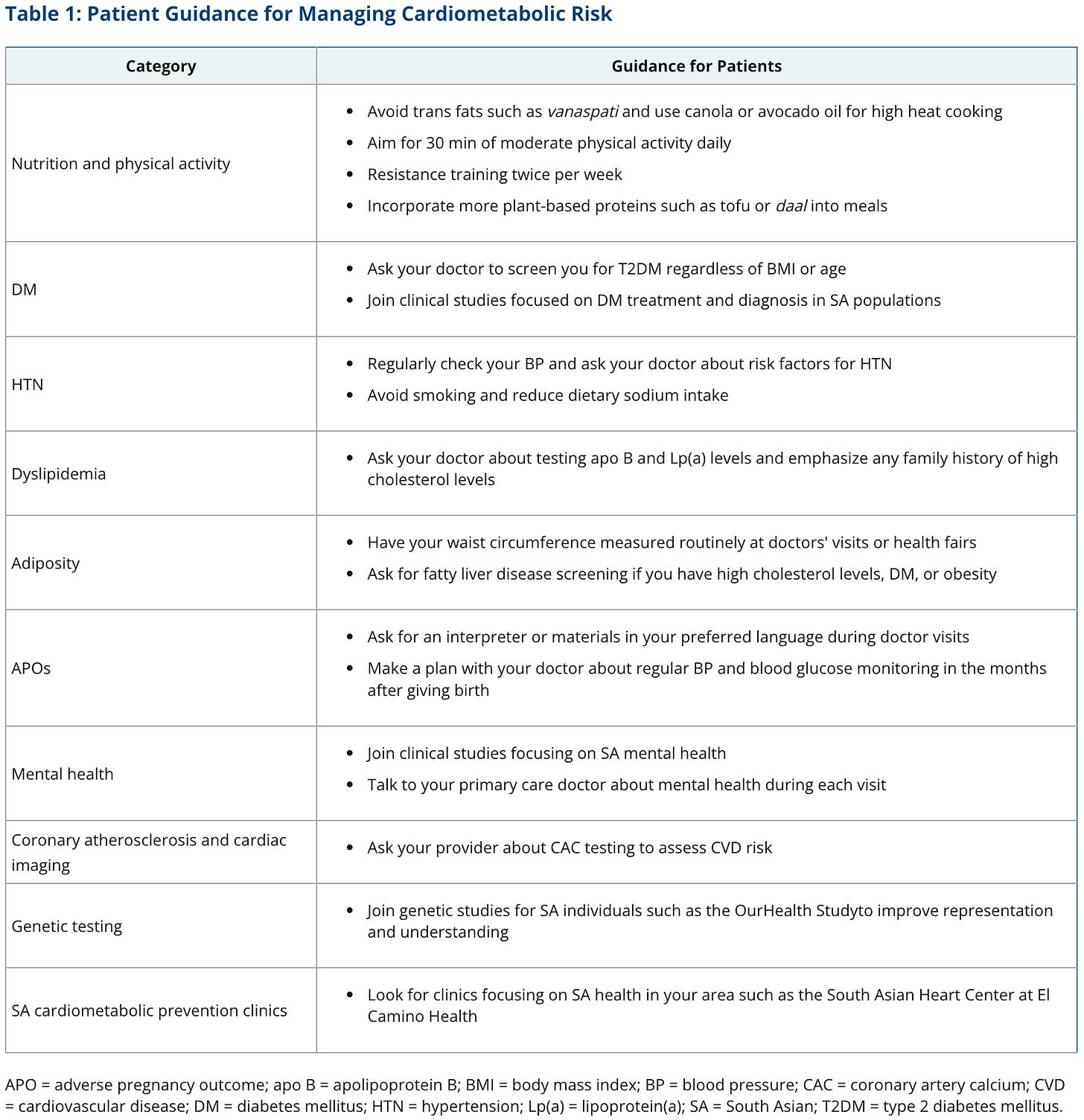
This paper is a comprehensive roadmap for clinicians, communities, and academia. It synthesizes the unique risk factors South asians face, from diet and adiposity to genetics, mental health, and adverse pregnancy outcomes and proposes a framework for action.
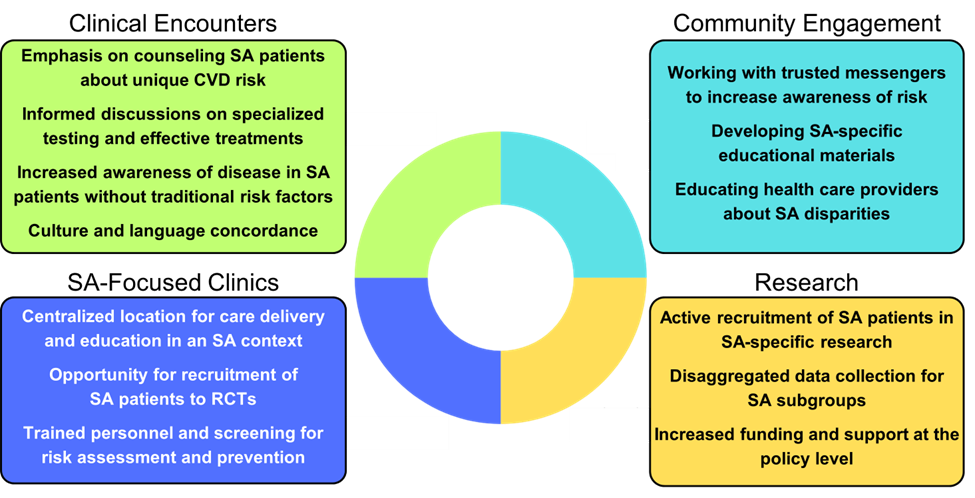
The paper organizes its recommendations across four key domains: Clinical, Community, Research, and Policy. This multi-pronged approach (which they illustrate in the chart below) aims to build a new, integrated system of care that moves from simple awareness to tangible, large-scale intervention.
What I Liked
Advanced Lipids Front and Center: The guidelines finally and officially recommend testing for Apolipoprotein B (ApoB) and Lipoprotein(a) (Lp(a)). This is a massive win. It (finally!) moves us beyond basic LDL-C and acknowledges that for South Asians, particle count (ApoB) and genetic risk (Lp(a)) are the real metrics that matter for identifying our hidden risk.
A Call for Dedicated SA Clinics: Something we’ve seen emerging nationally especially in higher density populations. The paper calls for establishing South Asian Cardiometabolic Prevention Clinics. This is a critical and necessary step. A generic primary care setting is often insufficient for the comprehensive, culturally-specific care we need.
The AI & Data Frontier: My own addition to their point: these clinics shouldn’t just be centers for care, but centers for data. They create the perfect infrastructure to build a complimentary data layer, allowing us to train AI models and risk calculators specifically on South Asian physiology.
Focus on Clinical Trials: The paper correctly identifies that South Asians are a “void” in clinical trial data. It highlights trials like SAHELI and SAHARA as a starting point, which is crucial. We cannot create evidence-based protocols for our community without data from our community.
What I Found Lacking
Premature Focus on CAC Scores: The inclusion of Coronary Artery Calcium (CAC) testing feels early. CAC only measures calcified plaque, while many South Asians suffer heart attacks from non-calcified, vulnerable soft plaque that a CAC scan can miss. A score of zero might give a false sense of security, and we should be prioritizing markers of inflammation (hs-CRP, OxLDL) and endothelial dysfunction first.
Missed Opportunity on Insulin Resistance: The paper rightfully flags our high diabetes risk but stops short of recommending advanced, early-stage diagnostics. For a population with profound insulin resistance, we must be looking at Fasting Insulin, HOMA-IR, and C-Peptide to catch metabolic dysfunction before it becomes diabetes. It also misses the vital role of Continuous Glucose Monitor (CGM) data to spot the post-meal (post-prandial) spikes that HbA1c averages out.
The Mitochondrial & Inflammatory Blind Spot: This is the biggest void. The framework fails to address the root cause of our phenotype: mitochondrial dysfunction and chronic low-grade inflammation. Clinically, at our own practice, we see clear signs of mitochondrial dysfunction (e.g., in energy production, oxidative stress) long before they manifest as the high-risk lipid numbers this paper focuses on. This dysfunction is the initial spark for cardiometabolic disease, and ignoring it means we’re only catching the fire after it’s already spread.
For a population whose cellular engines are inefficient, a truly comprehensive guideline must include protocols for assessing and supporting mitochondrial health.
This is a critical research frontier, and we need studies on everything from lifestyle interventions to complimentary therapeutics like peptides (SS-31, MOTS-c, Humanin) that could support our unique mitochondrial framework.
Which is why we at Cellspan Health, have built a comprehensive collection of current literature and studies on mitochondrial health and interventions to offer our patients all options in improving their mitochondrial health. (Feel free to reach out if interested in our NotebookLM for South Asian mitochondria. Here is guide to NotebookLM that I made.)
The Grasshopper Verdict
This ACC/ASPC guideline is a foundational piece. It’s a necessary public acknowledgement of our unique health crisis and provides the clinical tools, like ApoB and Lp(a) testing, to make an immediate difference in diagnosis. It’s a powerful building block.
Now, the work shifts to physicians: to push our clinicians, researchers, and communities to fill the void. We must advocate for trials, prioritize sophisticated metabolic screening (like HOMA-IR, hs-CRP, and CGMs), and start talking openly about the role of mitochondrial fitness and inflammation in South Asian longevity. More is needed,and now.
This is our opportunity to help the community move from generalized, passive risk management to targeted, proactive, and culturally informed health optimization.
— Omar