The Migrant Microbiome
Dysbiosis and Changing Gut of the South Asian Diaspora
We are doing a 3-part deep dive on the South Asian gut, starting with the gut microbiome, the gut-mitochondrial and gut-brain axis. Part 1 of 3 is below.
We often think of migration as a change of address. A new city, a new climate, new neighbors.
But biologically, it is a much more profound event…closer to a change of species.
Within months of arrival in the West, the internal ecosystem you inherited, the trillions of bacteria that co-evolved with your ancestors over millennia, begins to collapse. And with it, a cascade of dysfunction that helps explain why we face diabetes, heart disease, and autoimmunity at rates that defy every standard guideline.
We have explored the genetic angles of the South Asian paradox in previous posts: the fragile engine of our beta cells, the ghrelin dysfunction that strips our muscle, and the adiponectin deficit that makes every calorie dangerous. But genetics alone cannot explain the velocity of the change. Genes take generations to shift. Our health often deteriorates within a single generation of arrival.
The missing variable, or one big oen, is the gut microbiome. And its collapse is faster, and more reversible, than anyone realized.
The 6-Month Cliff
The loss of your ancestral microbiome doesn’t take decades. It takes months.
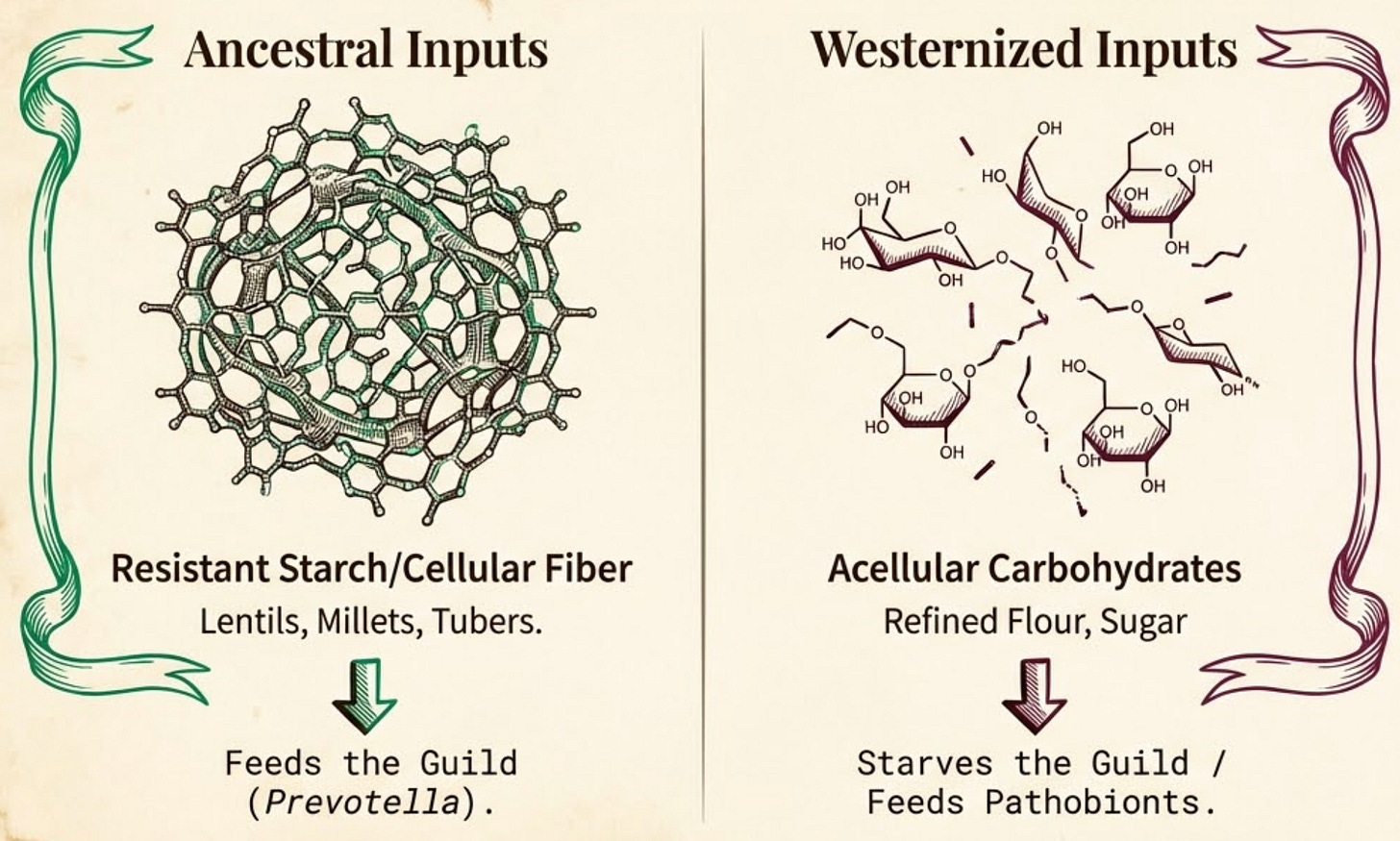
Landmark studies tracking immigrants reveal that significant displacement of native gut bacteria occurs within the first 6 to 9 months of residence in the West. In rural South Asia, the gut is dominated by Prevotella species; bacteria exquisitely adapted to break down the complex fibers in lentils, millets, and traditional vegetables into Short-Chain Fatty Acids (SCFAs), like butyrate.
Butyrate is not just fuel for the gut lining; it is an epigenetic signal. It works by inhibiting Histone Deacetylases (HDACs), effectively “switching off” the genes responsible for inflammation. When we lose Prevotella, we lose this critical chemical brake on our immune system.
Upon migration, Prevotella is rapidly displaced by Bacteroides, bacteria that thrive on animal proteins, fats, and refined sugars. While Prevotella may not disappear entirely, this represents a functional extinction of our dominant metabolic guild. The “keystone” species responsible for maintaining your gut barrier and feeding anti-inflammatory pathways are marginalized.
The substrate they depended on, the dal, the unpolished rice, the fibrous saag, has been replaced by ultra-processed foods that now constitute nearly 60% of daily calories in the standard Western diet.
Losing The Good Stuff
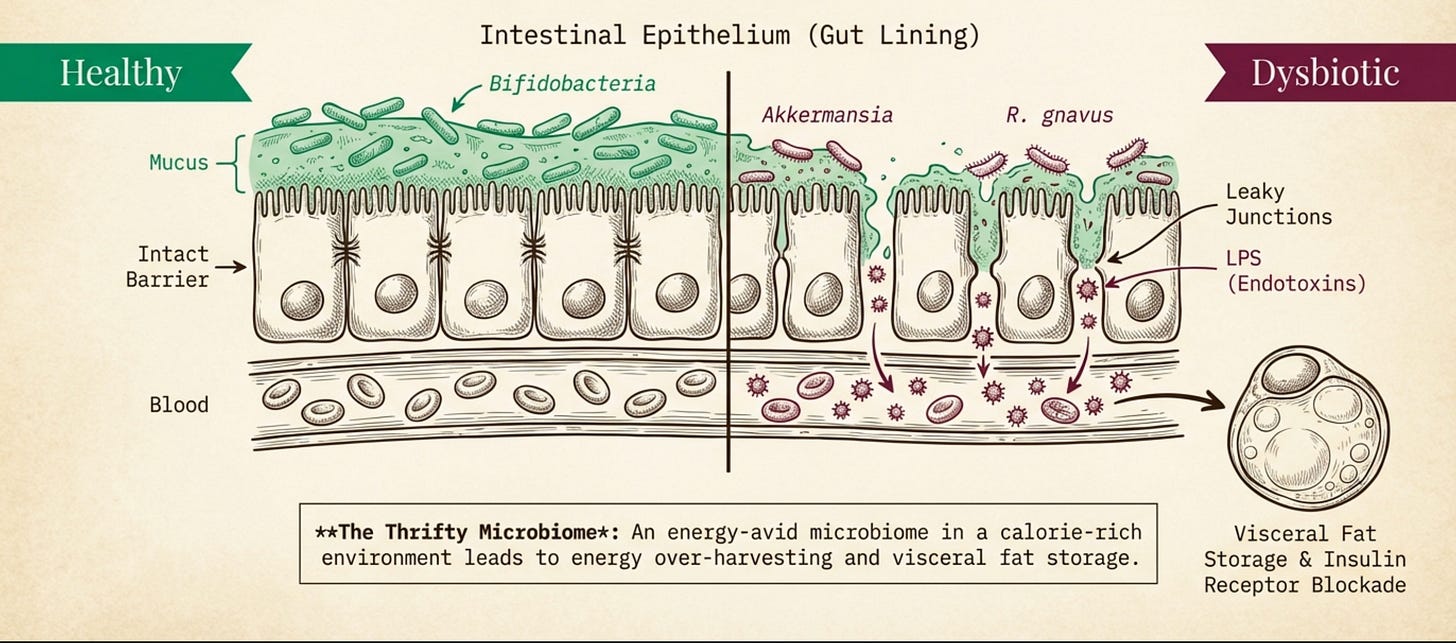
While Prevotella is the workhorse of digestion, Bifidobacteria are the guardians of the gut barrier. Research confirms that the traditional Indian microbiome carries significantly higher levels of Bifidobacterium, sustained by plant fibers and traditional fermented dairy, homemade dahi, lassi, idli, dosa, achaar, kanji.
In the West, this population crashes, contributing to a broader loss of overall microbial diversity.
The reasons are straightforward: beneficial bacteria need specific fibers to survive. When we swap whole dals for refined flour, we starve them. And the “yogurt” we replace dahi with is often pasteurized and standardized into weak monocultures that don’t colonize, and frequently loaded with sugar that feeds harmful bacteria instead.
When diversity drops, the gut lining weakens.. Bacterial toxins (lipopolysaccharides [LPS in above image]) escape into the bloodstream, triggering the chronic low-grade inflammation that drives insulin resistance. This is the same metabolic endotoxemia we discussed in the context of the flooded engine, except now we see where the flood originates.
As much as I love Straus…we may need to reprioritize.

The Mechanism: The False Alarm (TLR4)
These escaped toxins don’t just float around; they dock onto Toll-Like Receptor 4 (TLR4) on your immune cells. This receptor is designed to detect severe bacterial infections. When activated by a leaky gut, it tricks your body into thinking it is fighting septic shock.
The body responds by initiating a “war protocol”: it raises systemic inflammation and blocks insulin receptors in muscle and fat cells. Why? To keep blood sugar high so the immune system has fuel to fight the “infection.” This is one powerful mechanism by which a leaky gut drives Type 2 Diabetes, even in thin individuals.
“Westernized Vegetarian”
Many of us retain our vegetarian identity in the West, we may think this protects us.
It doesn’t. Not automatically.
The quality of the vegetarian diet often shifts dramatically. We replace complex, cellular fibers from traditional foods with “acellular” refined carbohydrates, white flour, polished rice, sugar. Worse, we introduce a flood of Omega-6 rich vegetable oils common in processed Western foods.
A “Westernized Vegetarian” diet, high in refined carbs and seed oils, low in complex fiber; can be ecologically worse for the South Asian microbiome than a moderate omnivorous diet. It creates fermentable substrate for gas-producing bacteria (the bloating we all know too well) without feeding the species that protect our metabolic health.
Enzymatic Extinction
Perhaps the most alarming finding is the loss of CAZymes, the molecular “scissors” our bacteria use to break down plant fibers.
Studies on South Asian Canadians show that second-generation immigrants often completely lack the genes required to degrade specific traditional fibers. This means even if you try to revert to a high-fiber ancestral diet later in life, your gut may no longer possess the machinery to process it efficiently.
This creates a vicious cycle. We avoid fiber because it causes discomfort, further starving the few remaining beneficial bacteria.
Dysbiosis and The Metabolic Mismatch
How does this connect to diabetes?
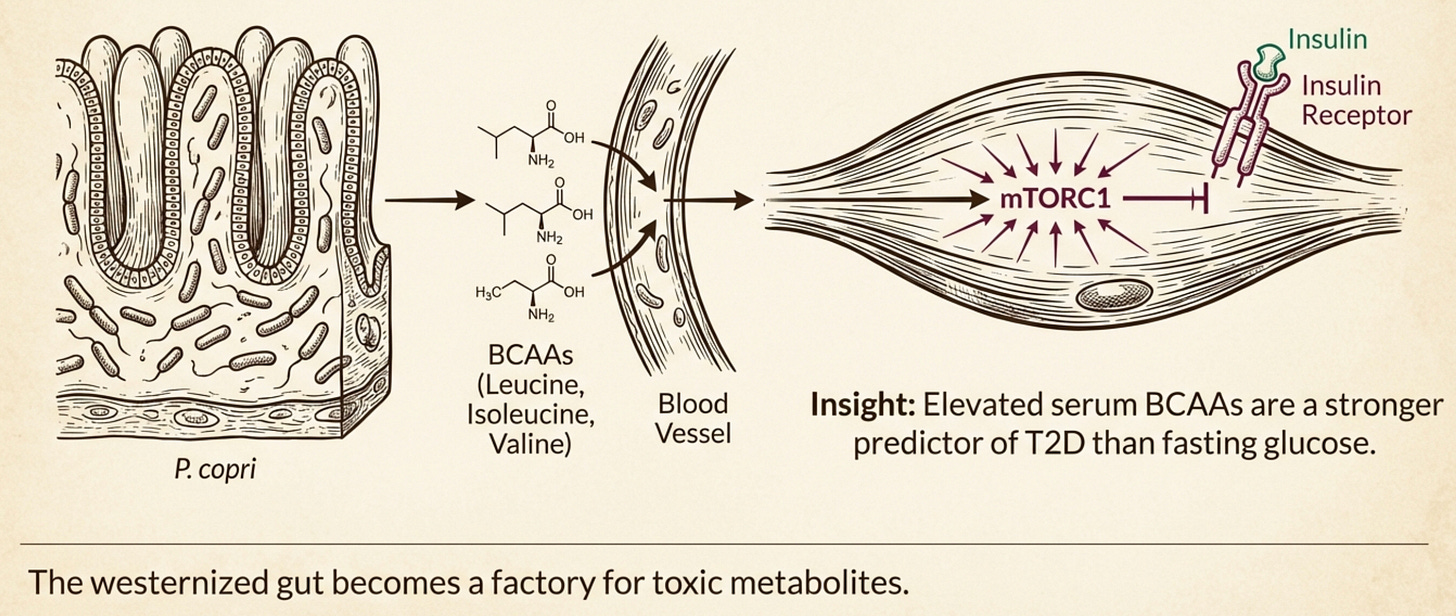
Dysbiotic gut bacteria (specifically certain strains of P. copri and Bacteroides) are prolific producers of Branched-Chain Amino Acids (BCAAs). As detailed in this pioneering metabolic research, elevated serum BCAAs are a potent driver of insulin resistance.
Recent research points to specific strains of Prevotella copri and Bacteroides as culprits here. It is important to note the nuance: P. copri is not universally “bad,” some strains found in traditional rural diets are beneficial. However, the specific strains, as seen in the Danish study above, that tend to thrive in the Westernized gut are frequently linked to BCAA production and insulin resistance.
The westernized South Asian gut becomes a factory for these metabolites, effectively blocking insulin signaling in your muscles and driving visceral fat storage, even if you aren’t overeating.
Second Generation Gets Hit Worse
The most profound impact is seen in the second generation.
First-generation immigrants often retain a “transitional” microbiome, a shadow of their ancestral gut that provides some residual resilience. But Gen 2, born in the West, faces something worse: complete extinction of ancestral heritage microbes from birth.
Born into sterile hospital environments, often via C-section (which bypasses the critical seeding of maternal vaginal flora), and exposed to higher rates of antibiotics in early childhood, Gen 2 children possess a microbiome nearly indistinguishable from the general Western population.
They have the South Asian genome. But the Western microbiome. From day one.
The Mechanism
Our immune cells rely on specific ancestral bacteria (our “Old Friends”) to train a specialized squadron of immune cells called Regulatory T-Cells (Tregs). Tregs are the peacekeepers; their job is to tell the immune system when not to attack.
Without early exposure to diverse microbes, the immune system fails to produce enough Tregs. It remains “uneducated” and trigger-happy.
This mismatch is driving an explosion of autoimmunity in younger generations:
Inflammatory Bowel Disease (IBD): Once vanishingly rare in South Asia, conditions like Crohn’s and Ulcerative Colitis are skyrocketing in the diaspora. In Canada, South Asian immigrants now have one of the fastest-growing rates of IBD in the country, often presenting with more aggressive disease than Caucasians.
The Skin-Gut Axis: Eczema and psoriasis are often the first visible signs of this. These aren’t just “skin conditions,” they are external signals of a gut barrier that has lost its integrity.
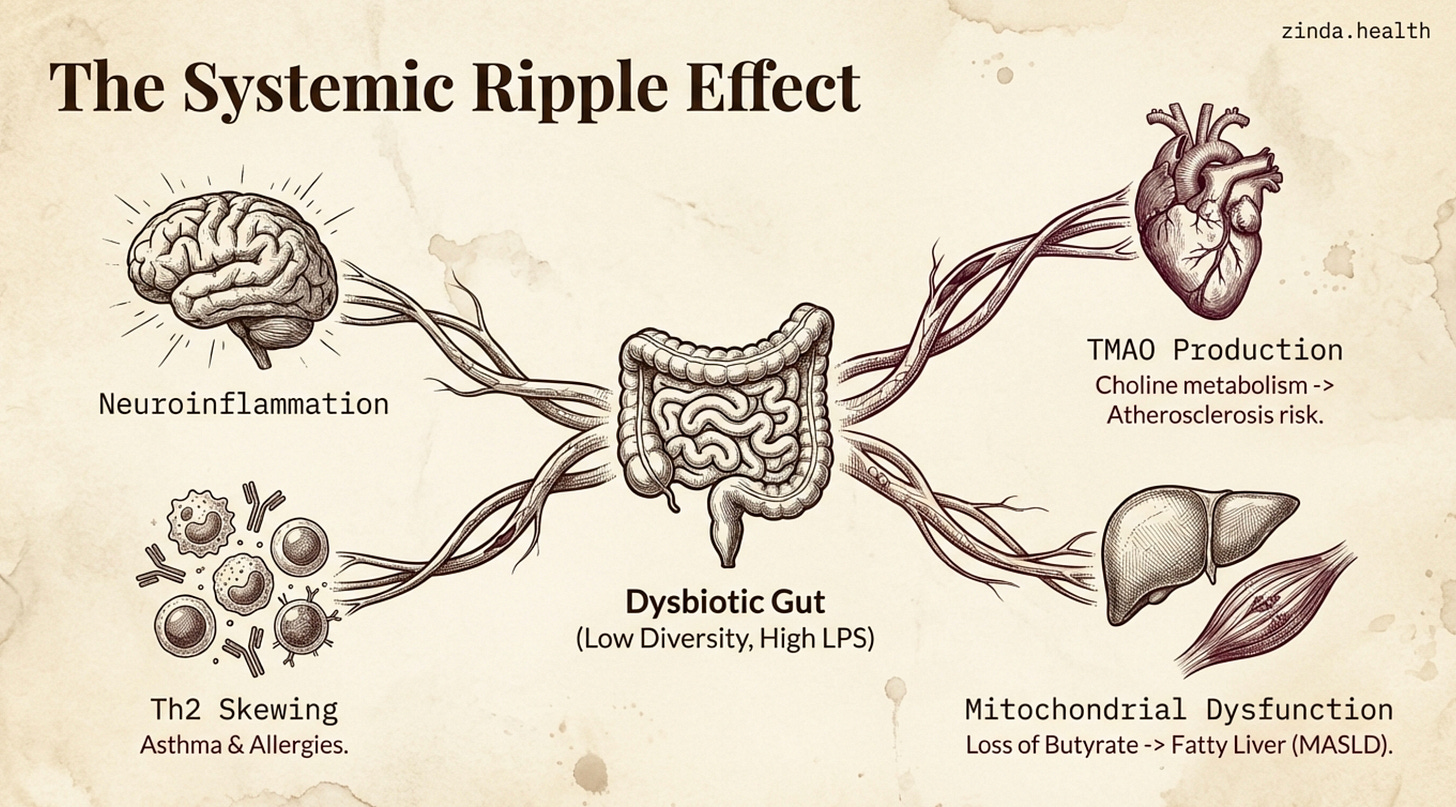
Asthma & Allergies: Asthma rates in diaspora children have surged, often surpassing their non-immigrant peers.
Gut-Brain Connection
As we already know well about the Gut-Brain Axis, a mention on its impact.
The gut produces roughly 90% of your body’s serotonin, the neurotransmitter that regulates mood, sleep, and gut motility. This process depends heavily on microbial metabolites.
When the gut is inflamed and dysbiotic, something shifts. Pro-inflammatory signals commandeer the pathway that makes serotonin and divert it toward producing neurotoxic compounds instead. The result is a double blow: less serotonin for your brain, plus inflammatory metabolites that cross the blood brain barrier.
This helps explain why South Asian immigrants, already facing acculturation stress, family separation, and discrimination, may have a lower biological threshold for depression and anxiety. One in five US South Asians reports experiencing a mood disorder in their lifetime. The gut isn’t the only factor. But it is a significant one that rarely gets discussed.
Reclaiming the Internal Ecosystem
The situation is urgent, but not hopeless.
Understanding that our health issues are ecological rather than just genetic gives us a new lever for change.
Feed the guild. Prioritize complex, cellular fibers, whole mung beans, steel-cut oats, fibrous vegetables. Not “whole wheat” flour.
Revive the Bifido-Shield. Don’t rely on sweetened store bought yogurt. Reintroduce traditional fermented foods, homemade 24-hour fermented dahi, idli/dosa batters fermented naturally, kanji.
Filter the oils. Eliminate high Omega-6 vegetable oils in favor of traditional fats (ghee, mustard oil) or olive oil.
A Note on Reversibility: Reclaiming your biome is possible, but reversibility has limits. Some microbial extinctions in the second generation can be permanent. This makes early intervention, especially for children, critical.
Migration changed our biology. It is up to us to adapt our lifestyle not just to fit the country we live in, but to respect the ancient ecosystem we carry within us.
But this is only part of the story.
In Part II, we will follow where these gut toxins travel next, directly to your mitochondria, the power plants of every cell in your body. And we will explore why fixing the gut might be the first step to fixing your energy, your metabolism, and your longevity.
This is Part I of a three-part series on the South Asian gut. As always any feedback is greatly appreciated. Please share with those you think would enjoy this.
-Omar