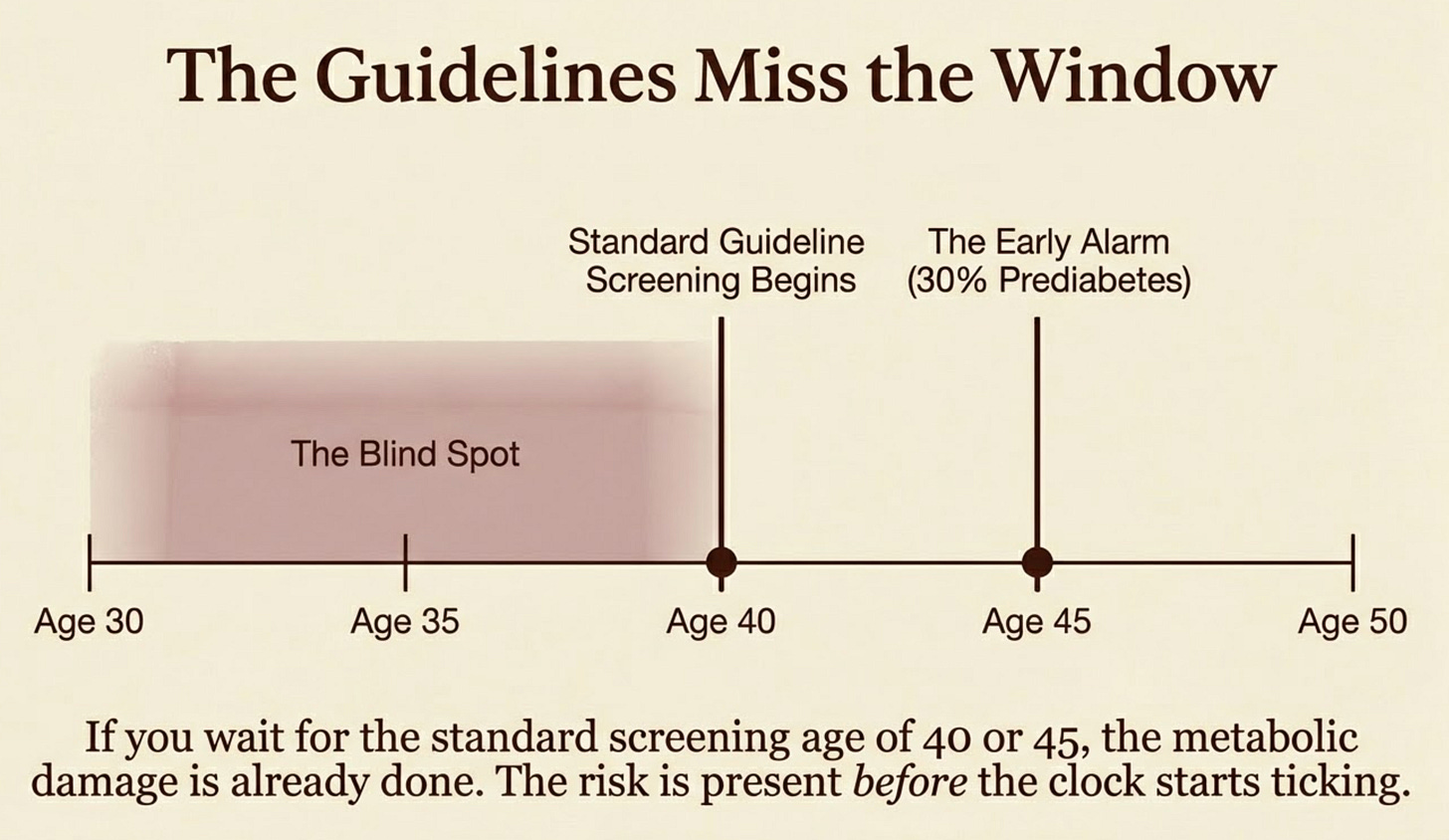
Chai Shots #007: The Early Alarm
Pre-diabetes comes early for South Asians
Welcome back to Chai Shots, our series on reviewing the most important research in South Asian health optimization.
A new study in the Journal of the American Heart Association study shed valuable insights on prediabetes in South Asians in the US.
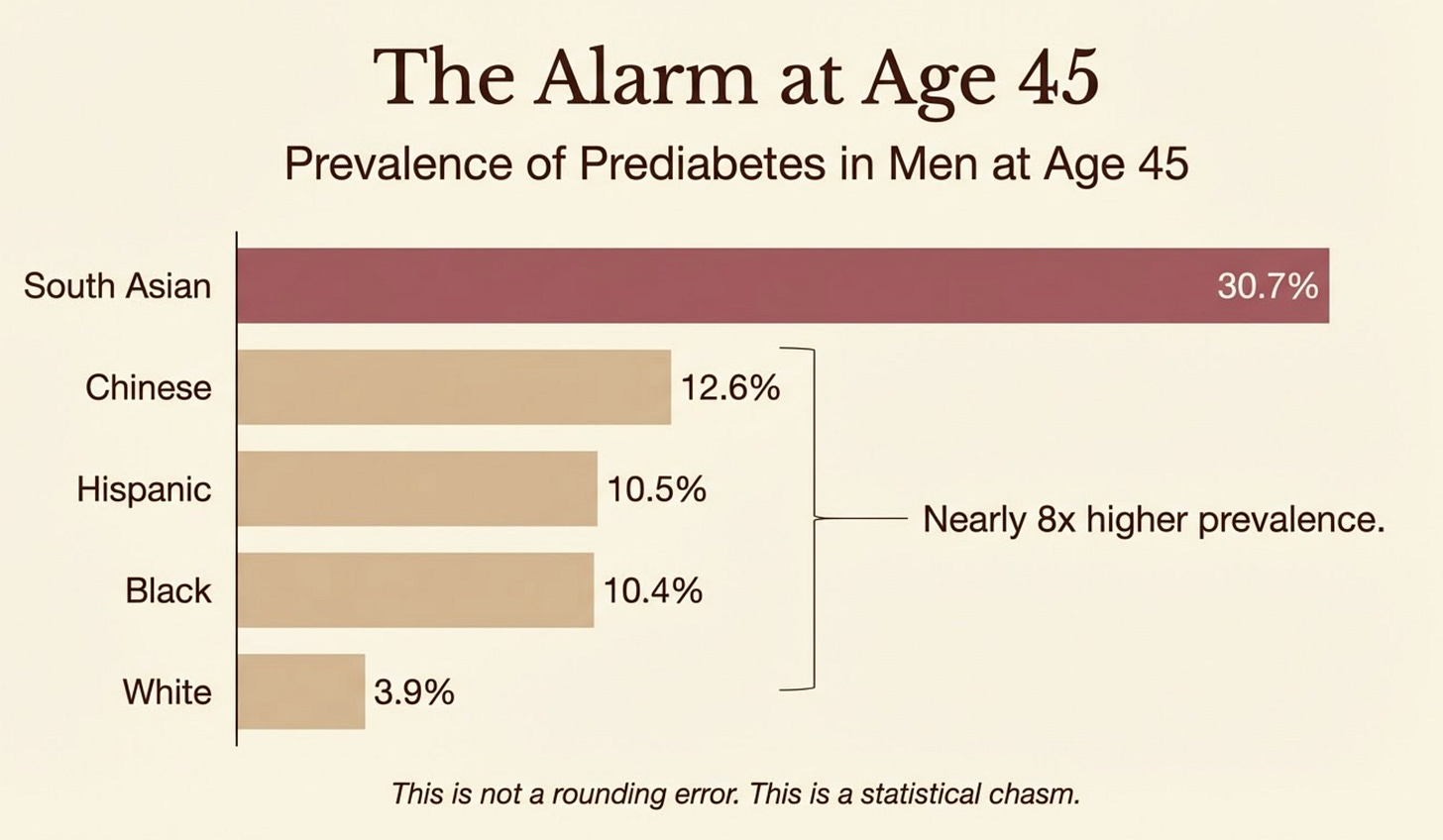
At age 45, South Asian men in the US have a prediabetes prevalence of 30.7% by study criteria (meaning we use fasting glucose between 100–125 mg/dL for everyone in the study).
White men the same age? 3.9%.
That 3.9% may feel low compared to national headlines (one would think this is higher considering the Standard American Diet (SAD)), and it is. Reason is this cohort was restricted to adults free of cardiovascular disease at baseline, which skews healthier than the general population.
The point isn’t the absolute numbers. It’s the ratio.
An eightfold divergence, in men who by almost every behavioral measure in this same study are doing better than their peers.
About the Study
Researchers from Northwestern and UCSF combined two landmark US cohort studies, MASALA (South Asian adults, a study we have referred to many times on this Substack) and MESA (White, Black, Chinese, and Hispanic adults), modeling clinical and behavioral risk factors across repeated exam cycles spanning midlife, from age 45 to 55, using approximately 2,700 participants.
This isn’t social media nutrition research. It’s the most thorough, detailed study on cardiac risk done on the diasopora to thsii day; repeated clinical examinations, labs, vitals, dietary assessments, used to ask a precise question: do South Asian adults develop cardiovascular risk factors earlier than other groups, and does that trajectory differ by gender?
The findings at age 45:
The good:
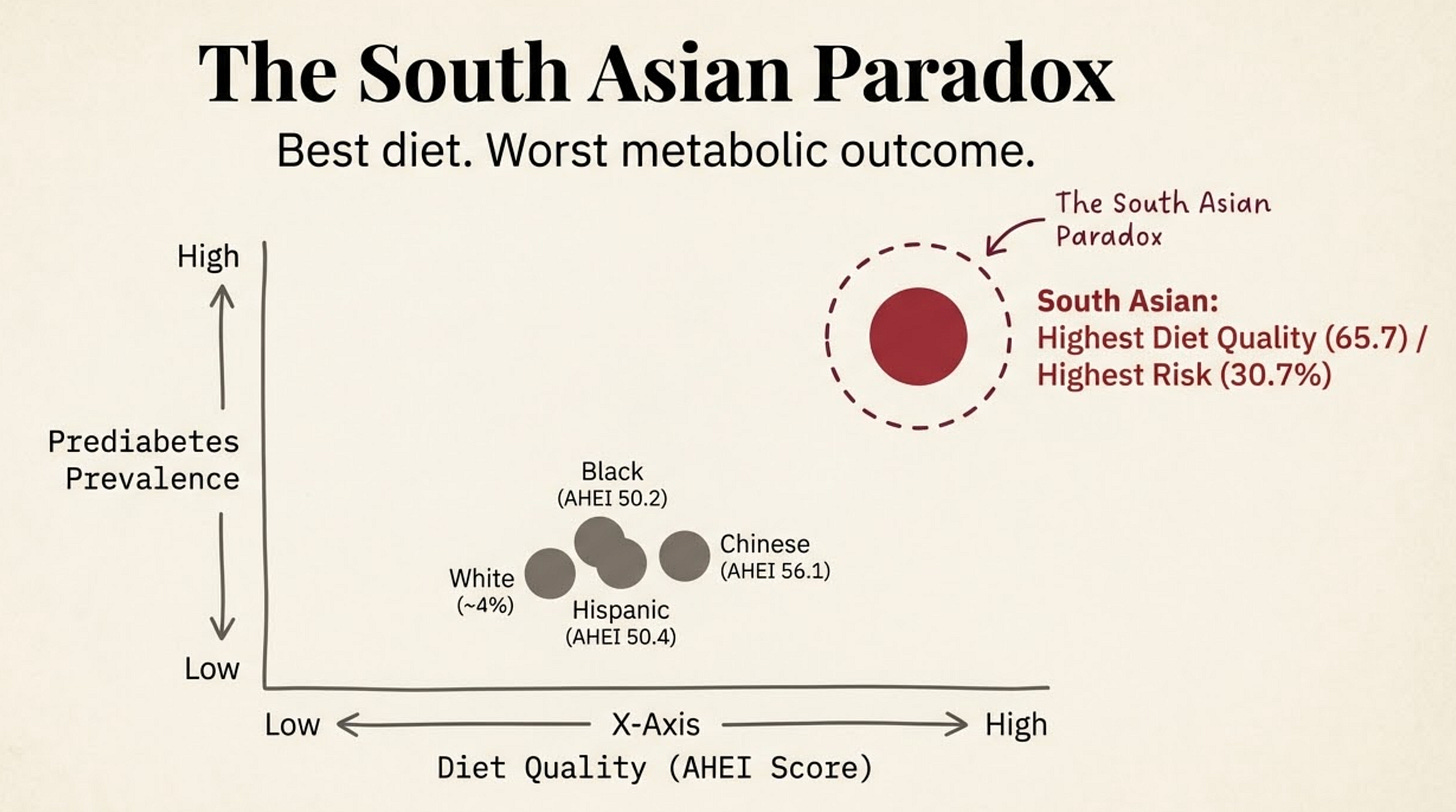
Highest diet quality scores of all groups, South Asian men scored 65.7, women 67.6 on the Alternative Healthy Eating Index, leading every other group by a substantial margin
Lowest alcohol use
The bad:
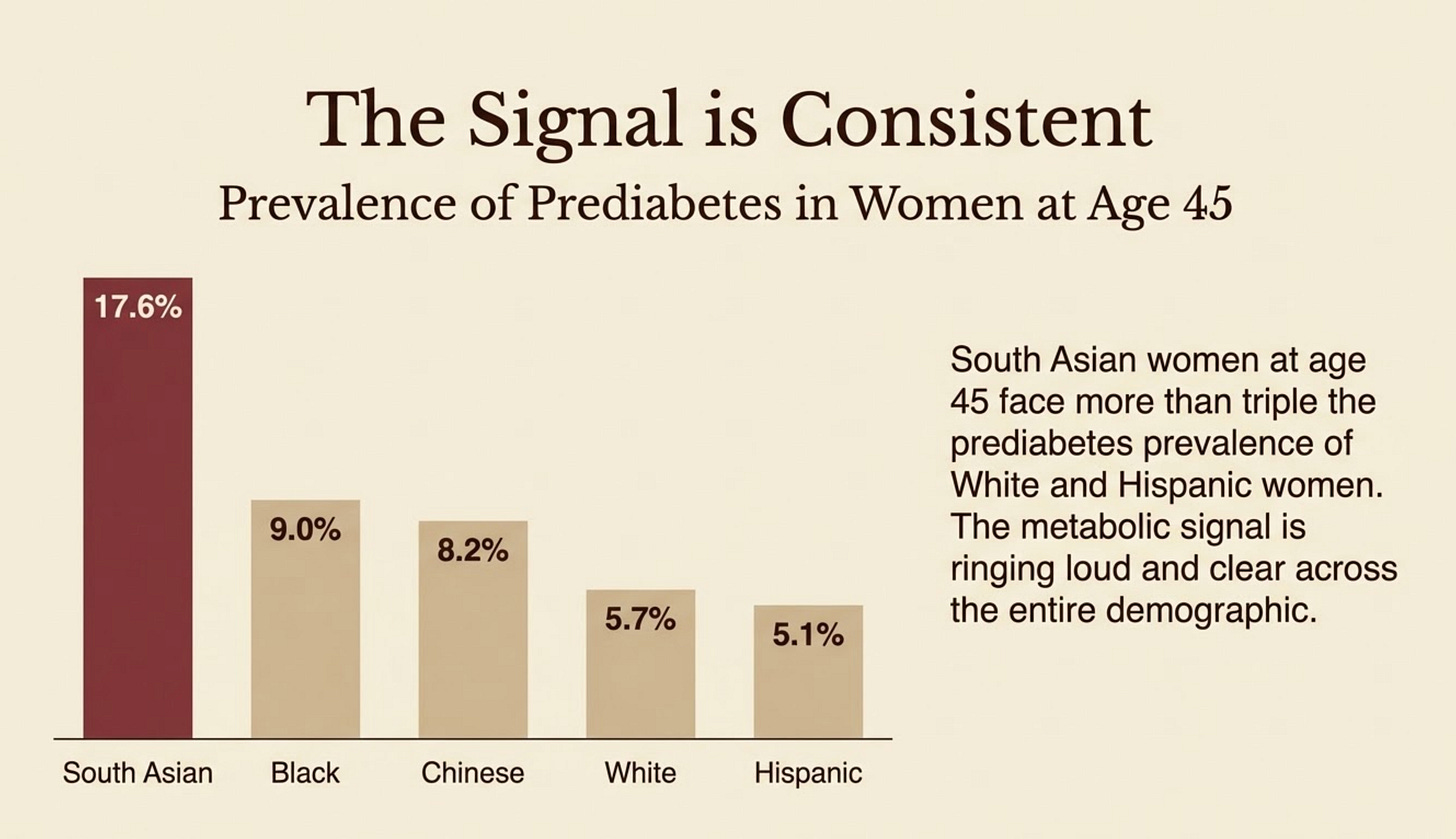
Highest prediabetes prevalence of all five racial and ethnic groups, in both men and women
Highest hypertension prevalence compared with White, Chinese, and Hispanic adults, only Black adults were comparable
Leading dyslipidemia rates among men compared with White, Chinese, and Black men
By age 55, the divergence sharpens.
South Asian adults had the highest probability of developing diabetes of any group.
“Our findings are consistent with previous studies demonstrating that South Asian populations develop diabetes at younger ages compared with non‐Hispanic White populations and even earlier than other Asian subgroups.”
South Asian men were nearly three times as likely to develop diabetes by 55 as White men. South Asian women saw prediabetes jump 18.5 points, from 17.6% to 36.1%, nearly double the increase of any other group in the study.
The authors named it themselves, and then offered an explanation that implicates not just physiology, but biography: "worse clinical risk factors despite a greater prevalence of protective behaviors" may stem from lifestyle exposures that preceded the study period entirely.
The lifestyle paradox isn’t a footnote. It’s the plot.
The Zinda Reading
This is where the Fragile Engine and the Overflow Tank do their quiet, relentless work.
A South Asian body at 45 is not a caucasian body at 45.
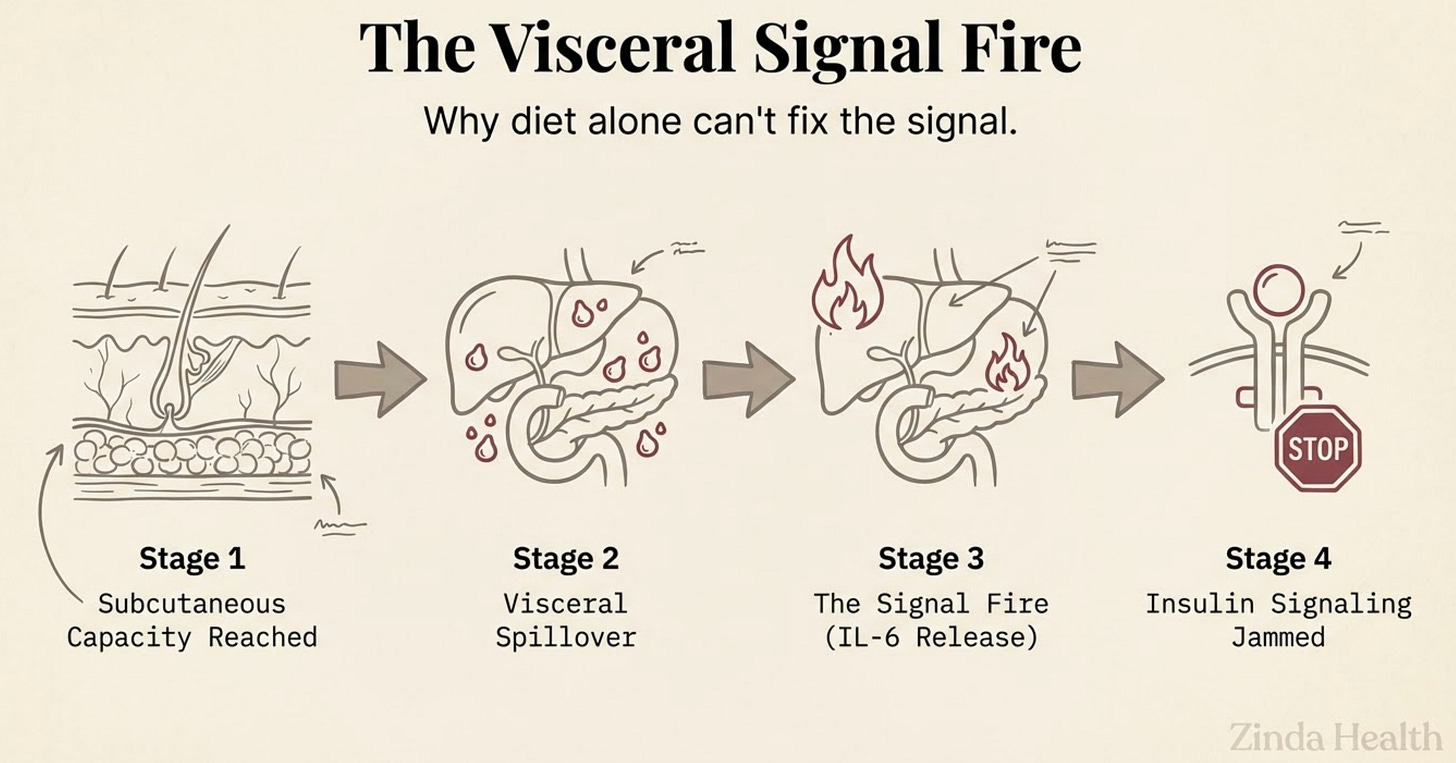
Beta-cell reserve runs smaller from birth, and subcutaneous fat storage saturates earlier. When the overflow goes visceral, into the liver and surrounding organs, the metabolic signal changes entirely. Visceral fat doesn’t just sit there. It behaves like an endocrine organ, pushing inflammatory signaling (IL-6 among others as we discussed here last month), that worsens insulin resistance even when the person eating the meal has the best diet score in the room.
This is why diet quality alone cannot move the needle the same way. The Fragile Engine was already running closer to redline before the fork and knife ever came into the picture.
But the paper goes further than biology. The authors offer an explanation that implicates not just our physiology but our biography.
Most middle-aged South Asian adults in the United States are immigrants. Many arrived eating the way people actually eat at home, fried snacks, sweets, high-fat dairy, limited structured exercise. Over years of assimilation, habits shifted. Better diets. More movement. The MASALA study itself found that women who integrated into American culture had more favorable metabolic profiles than those who maintained strict dietary and lifestyle separation (below).

So what we’re measuring at age 45 is not a lifetime of good behavior. In many cases, it’s a recent conversion. And the Fragile Engine doesn’t care that you started eating well at 38. It remembers the decades before.
The damage isn’t always happening now. Sometimes it happened earlier, in childhood, in the subcontinent, in the decade after immigration before the habits shifted. By the time a South Asian patient walk into a clinic at 45 with excellent diet scores and a prediabetes diagnosis, the story that produced that number may be 20 years old.
What the Guidelines Still Miss
Current ACC/AHA guidelines acknowledge South Asian ancestry as a cardiovascular risk-enhancing factor, but they don’t operationalize what that means for earlier metabolic screening in a way that actually matches this burden. Lp(a), ApoB testing, earlier fasting insulin, HOMA-IR, HbA1c tracked against lower thresholds, none of this is routine. South Asian ancestry is a flag in the guidelines. It hasn’t yet become a protocol.
The infrastructure for better care exists, but it’s uneven. SAHELI suggests culturally adapted programs can improve behaviors, even if cardiometabolic risk-factor changes versus written education were modest, meaning we may need earlier timing, higher intensity, or different targets (waist/visceral adiposity, insulin resistance), not just ‘better advice’.
A Note on What This Study Didn’t Say
The authors were careful on generalization of this data, as we should be. MASALA participants were recruited largely from Indian backgrounds, from two US cities. This is not the full South Asian diaspora. The study also couldn’t use genetically inferred ancestry or biological sex data, which limits mechanistic conclusions.
But the direction of the signal is clear. And it’s been pointing the same way for years, in MASALA, in UK Biobank, in Yajnik’s foundational thin-fat phenotype work. This isn’t a new alarm. It’s the same alarm, getting louder.
The question is no longer whether it’s ringing.
The question is whether anyone is listening, and whether we’re acting before the decade of drift becomes irreversible.
— Omar