GLP-1 and the South Asian Phenotype
Resistance, Miracle and a Warning
This is the third and final part of our discussion on the South Asian gut, part 1 and part 2 here. From here we will move on to the liver next week.
Feedback on topics always welcome!
At Zinda, we don’t care about the hype. We care about the phenotype.
Nothing has garnered hype like GLP-1. Super bowl level hype.
For the South Asian community however, GLP-1s may be the most important medication, almost a miracle. It’s not just about fitting into a wedding outfit; it’s about correcting a fundamental evolutionary mismatch.
Lets get into it.
In our previous deep dives, we’ve explored the “Thin-Fat” Paradox, how South Asians suffer from metabolic disease at lower body weights than our Western counterparts. We’ve discussed our “Thrifty Genotype”, an evolutionary adaptation for starvation that has become a liability in the age of abundance. And over the last month delved into the South Asian gut, how its lining, microbiota and axis form a circuit incongruous to a diaspora.
Today, we are connecting those dots, all seemingly leading toward GLP-1s and why they could be metabolic correctors ideal for the specific bottlenecks in the South Asian phenotype.
GLP-1s 101
Before we dive into the South Asian specifics, let’s strip away the brand names and look at the molecule fundamentally.
GLP-1 (aka Glucagon-like Peptide-1) is an incretin hormone naturally produced in your gut after you eat. Like most peptides, they are signaling molecules, messengers who instruct the target cell/organ to do something. In the case of GLP-1s, it communicates between the gut and the rest of the body.
When you eat a meal, GLP-1 travels through your system to coordinate a complex physiological response:
In The Brain: It binds to receptors in the hypothalamus to shut down “food noise” that constant mental chatter asking “What’s for dinner?” while you’re eating lunch.
In The Stomach: It slows gastric emptying, keeping you physically fuller for longer.
In The Pancreas: It primes the beta-cells to release insulin, but crucially only when glucose is elevated. This “glucose-dependent” mechanism is why it rarely causes dangerous lows (aka hypoglycemia), unlike older drugs (though risks increase if combined with insulin or sulfonylureas).
In The Liver: It suppresses glucagon secretion from pancreatic alpha cells, thereby stopping your liver from dumping stored sugar into your bloodstream unnecessarily.
For many people, this reads like weight loss. For South Asians, it can function more like metabolic triage, because the bottleneck is earlier, and the margin for error is smaller.
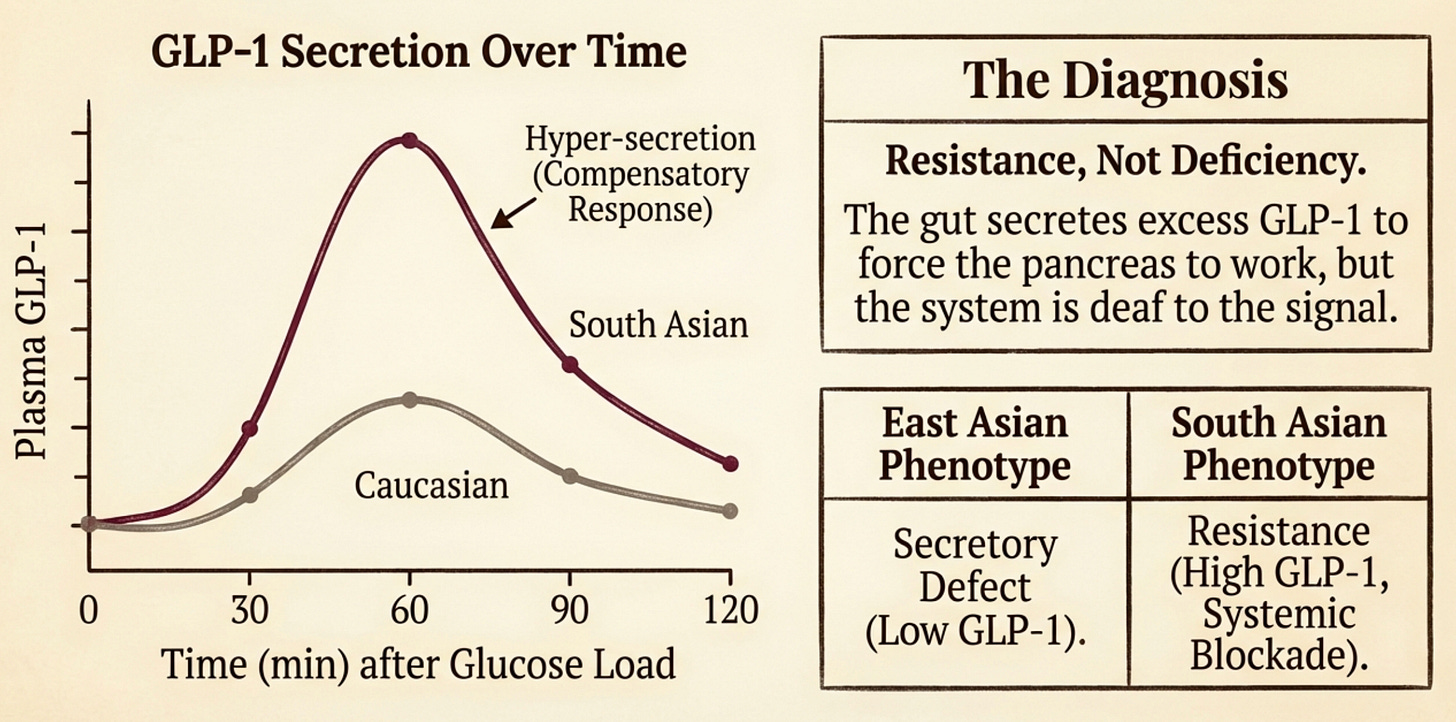
Resistance, Not Deficiency
When we talk about metabolic health, we obsess over insulin. We track spikes, we fear resistance, and we measure fasting levels. But insulin is just the soldier; it follows orders. We are slowly learning the real commanders are the incretins, hormones like GLP-1 that dictate how your body handles a meal.
Now, you might assume that because South Asians get diabetes earlier and more aggressively, we simply lack these hormones. The reality is the exact opposite.
Research comparing healthy young South Asians to Caucasians found a fascinating paradox: in response to sugar, South Asians actually secrete significantly higher levels of GLP-1.
Why?
Think of it as a scream for help. Your body “senses” the metabolic struggle, the insulin resistance in your liver and muscles, and the gut pumps out extra GLP-1 to force the pancreas to respond. But just like we are insulin resistant, we appear to be GLP-1 resistant.
Research strongly supports a “Compensatory Scream” hypothesis. Sleddering et al. (2014) found that healthy young South Asians secreted ~45% more GLP-1 (AUC) than matched Caucasians during a glucose challenge, yet still exhibited higher insulin resistance. This appears specific to our phenotype; Chong et al. (2022) showed that Indians produce significantly more GLP-1 than Chinese or Malays, directly correlating with metabolic dysfunction. Essentially, while the gut is working overtime to stimulate insulin (Misra, 2020), it is fighting a losing battle against systemic defects.
The signal is loud, but the body isn’t listening, a mismatch that suggests a distinct form of “GLP-1 resistance.”
This is why “natural” methods sometimes hit a wall and why pharmacological GLP-1s (which provide doses far higher than nature) can be so effective. They provide a signal loud enough to finally break through that resistance barrier.
Genomic Blind Spots
Research into the pharmacogenomics of GLP-1 agonists in South Asian populations is still in its infancy, especially as this is critical in understanding nuances of hyper-responders and poor responders. A large-scale genome-wide analysis identified a variant in the ARRB1 gene that is associated with an enhanced glycemic response to GLP-1 agonists. However, this variant is almost non-existent in individuals of Asian descent. Conversely, a common variant in the GLP1R gene was linked to a reduced response, but its specific frequency and impact within South Asian populations have not been clearly established.
The significant underrepresentation of South Asians in major clinical trials for these medications is a major obstacle to understanding the role of genetic factors in treatment response and a mission driven goal for Zinda.
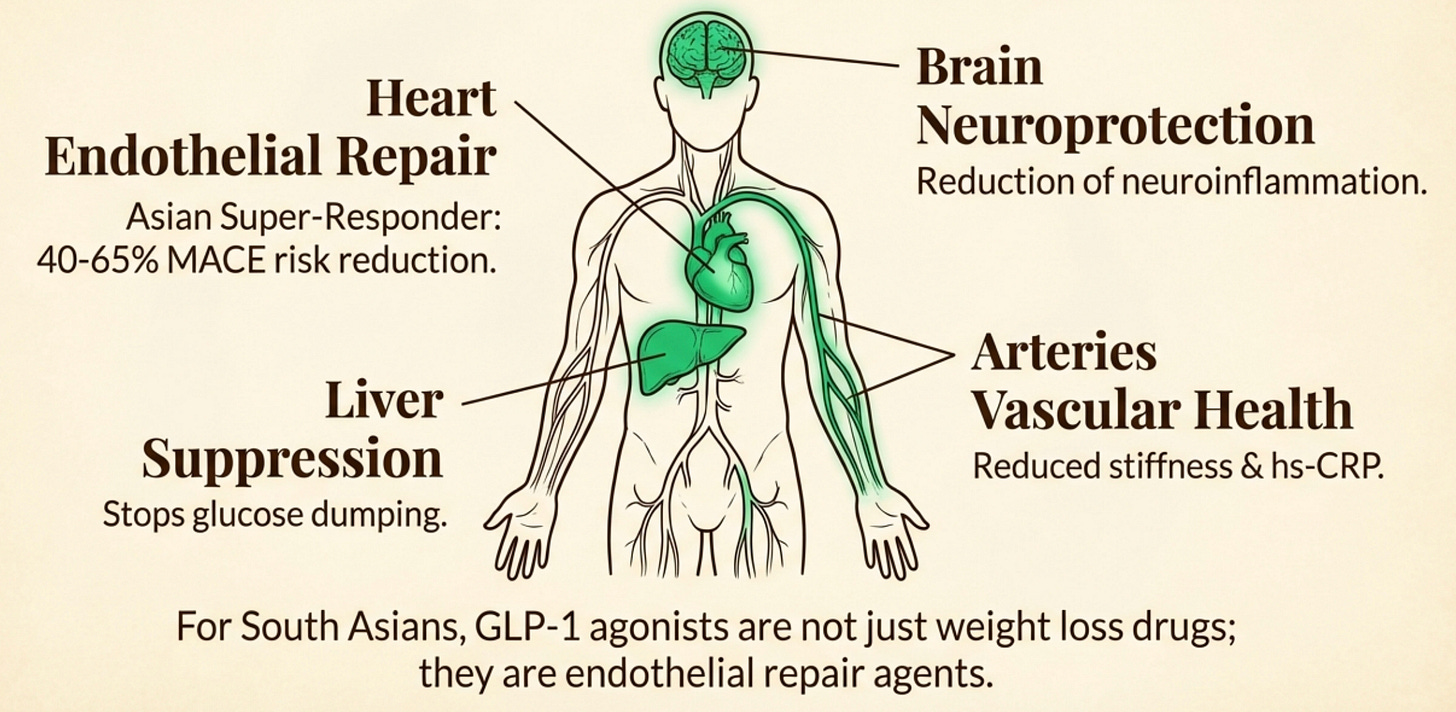
A Systemic Shield
One of the most important discoveries in recent years is that GLP-1 receptors are not just found in the pancreas or gut. They are ubiquitous, acting as a “systemic shield” for organs that are particularly vulnerable in the South Asian phenotype.
The Heart (Endothelial Repair): South Asians have some of the highest rates of premature cardiovascular disease. GLP-1 receptors line our blood vessels and the heart itself. Studies show that activation of these receptors improves endothelial function (the flexibility of blood vessels) and reduces arterial stiffness, often independent of weight loss.
Systemic Inflammation (The hs-CRP Connection): Chronic, low-grade inflammation is a hallmark of our phenotype, often visible in elevated hs-CRP levels even in “thin” individuals. GLP-1s appear to directly downregulate inflammatory cytokines. This is crucial because inflammation is the spark that often ignites the fuel of insulin resistance.
The Brain (Neuroprotection): Emerging research suggests GLP-1s reduce neuroinflammation. Given the links between insulin resistance and cognitive decline (often called “Type 3 Diabetes”), this offers a potential protective mechanism against neurodegenerative conditions like Alzheimer’s, which share metabolic roots with diabetes.
Why We Need to Rest, Not Whip
We have previously discussed the “Beta-Cell Fragility” of the South Asian phenotype. If the pancreas is a fuel tank, we are born with a smaller tank.
For decades, the standard treatment for diabetes in South Asia has been Sulfonylureas, older drugs that squeeze the pancreas to pump more insulin. In our framework, this is a mistake. It’s like whipping a tired horse; it works for a mile, but the horse collapses sooner.
GLP-1 receptor agonists work differently. They don’t just squeeze; they optimize.
They Rest the Beta-Cell: They only stimulate insulin when blood sugar is high, preventing the “burnout” that leads to early insulin dependence.
Pancreatic Offloading: By aggressively targeting visceral fat (the specific belly fat South Asians store), GLP-1s lighten the “trailer” significantly more effectively than Metformin.
Preservation: The goal isn’t just to lower A1c today. It’s to stop the beta cells from dying off so you don’t need injected insulin 10 years from now.
They Target the “Overflow”: The South Asian metabolic crisis is driven by ectopic fat, fat stored in the liver and pancreas because our subcutaneous (under skin) storage is limited. GLP-1s are exceptionally good at mobilizing this specific, dangerous visceral fat.
The Silent Epidemic
If there is one organ that defines the South Asian metabolic struggle, it is the liver.
South asians have some of the highest rates of MASLD (Metabolic Dysfunction-Associated Steatotic Liver Disease), often occurring in people who look “thin” or have a normal BMI. Recent studies in South Indian cities found a staggering 40% prevalence of fatty liver, much of it in non-obese individuals. This is “Lean MASLD,” and it is a silent killer. Because our subcutaneous fat storage (the safe fat under your skin) is genetically limited, any excess energy spills over almost immediately into the liver.
For South Asians, the liver becomes a bottleneck. Once it is clogged with fat, it becomes insulin resistant, pumping out sugar even when you are fasting, driving the cycle of diabetes.
This is where the every new generation of GLP-1s has shown leaping progress:
Semaglutide (Ozempic/Wegovy): Proven to significantly reduce liver fat, effectively “de-clogging” the filter.
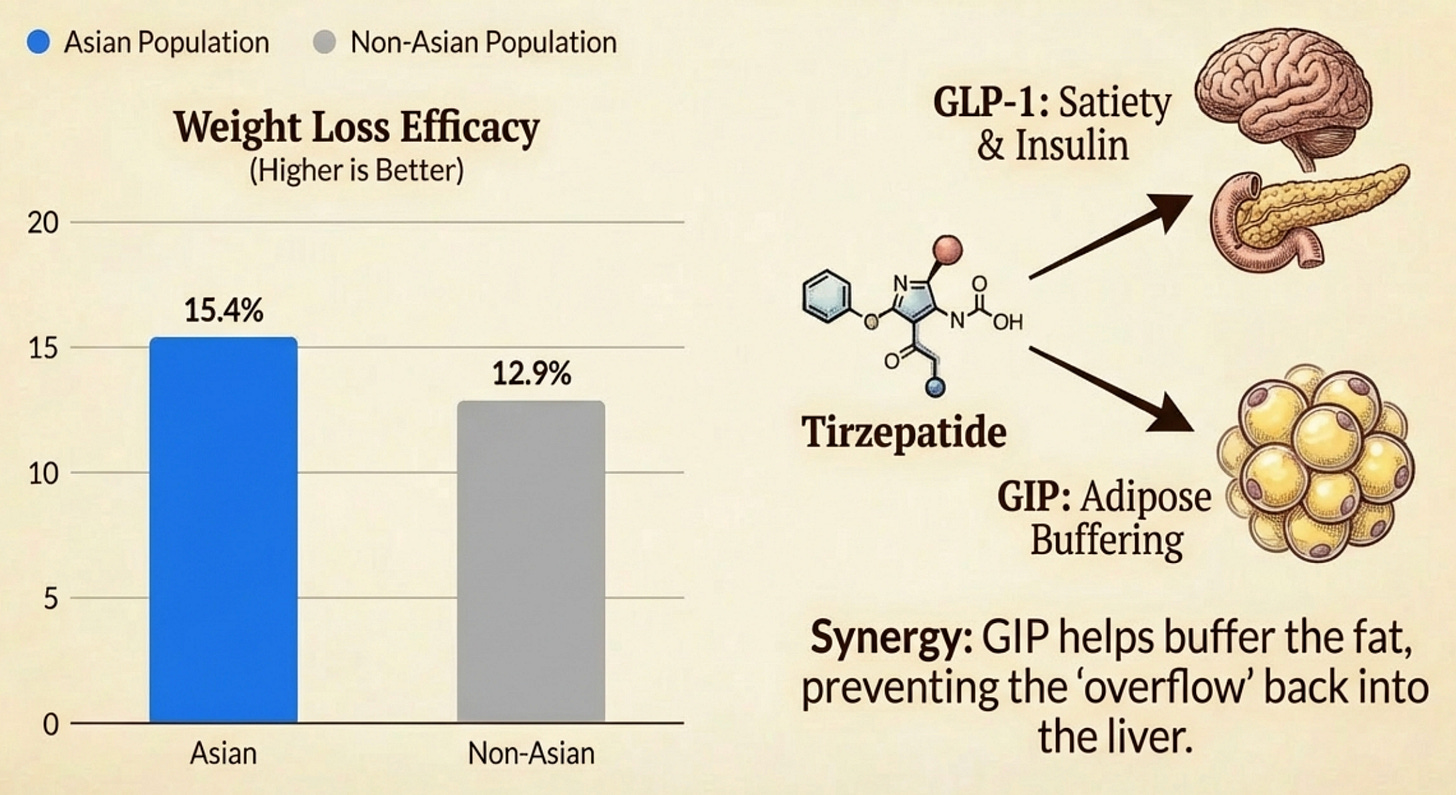
Tirzepatide (Mounjaro/Zepbound): This is a “dual agonist” (targeting GLP-1 and GIP). Early data, such as the SURPASS-3 MRI substudy, suggests it is even more potent for liver health, potentially halting the progression to fibrosis (scarring).
Retatrutide (The Future): I like to call this the liver GLP. This upcoming “triple agonist” (GLP-1, GIP, and Glucagon) is highly anticipated. In Phase 2 trials, it has shown the ability to resolve fatty liver in >85% of patients in just 48 weeks, with most patients dropping to normal (≤5%) levels. That is mind blowing as we have alwys assumed much of liver steatosis took years to improve. For a population prone to liver disease, this could be revolutionary.
Note: We will be doing a dedicated, comprehensive deep dive into MASLD and the South Asian Liver next week. Why this happens, why and how to screen early, much more... Stay tuned.
The Mitochondrial Connection
At Zinda, as most regular readers already know, we view metabolic health through the lens of bioenergetics, specifically, the mitochondria, our cellular engines. The South Asian “starvation-adapted” engine as we discussed in a previous Chai Shots post, is designed for efficiency, not capacity. When we flood it with modern “fuel oversupply” (processed carbs, seed oils), the engine gridlocks.
Emerging science suggests GLP-1s may help unclog this gridlock. They don’t just suppress appetite; studies indicate they may stimulate mitochondrial biogenesis, helping the body build more engines to burn through the lipid overload in our muscle cells.
The Muscle Trap
However, there is a critical nuance that we cannot ignore.
If you are South Asian, you are likely already battling sarcopenia (low muscle mass). It is a hallmark of our phenotype. GLP-1 medications cause weight loss, but without intervention, up to 40% of that loss can be lean muscle.
If you take these drugs and do not lift heavy weights, you risk becoming a smaller, weaker version of the “Thin-Fat” phenotype, lower weight on the scale, but a disastrously low metabolic rate and higher relative body fat.
Non-negotiables for GLP-1s:
Strength is Non-Negotiable: You must engage in resistance training to preserve the “thin” (muscle) while stripping the “fat”.
Protein Prioritization: Our traditional diets are often protein-deficient. On these medications, appetite drops, making it even harder to hit protein targets. Conscious, high-protein intake is medicine.
Know Your Liver Status: Before starting, understand your baseline. If you have “Lean MASLD,” these medications may be doubly effective for you, acting as both metabolic correction and liver therapy.
A note on stigma
Something I encounter with many South Asians patients is apprehension stemming from rumors, stories and stigma around these medication. It almost feels they are cheating physiology. For South Asians, GLP-1s are not “cheating.”
In our community, there is often a heavy stigma attached to medication, viewing it as a failure of willpower or a sign of weakness. We need to kill this narrative. Using a GLP-1 to correct a genetically entrenched resistance is no more “cheating” than wearing glasses to correct poor eyesight. It is a tool to level a playing field that evolution tilted against us.
Furthermore, we must shift our mindset from reactive to proactive.
When to Have the Conversation
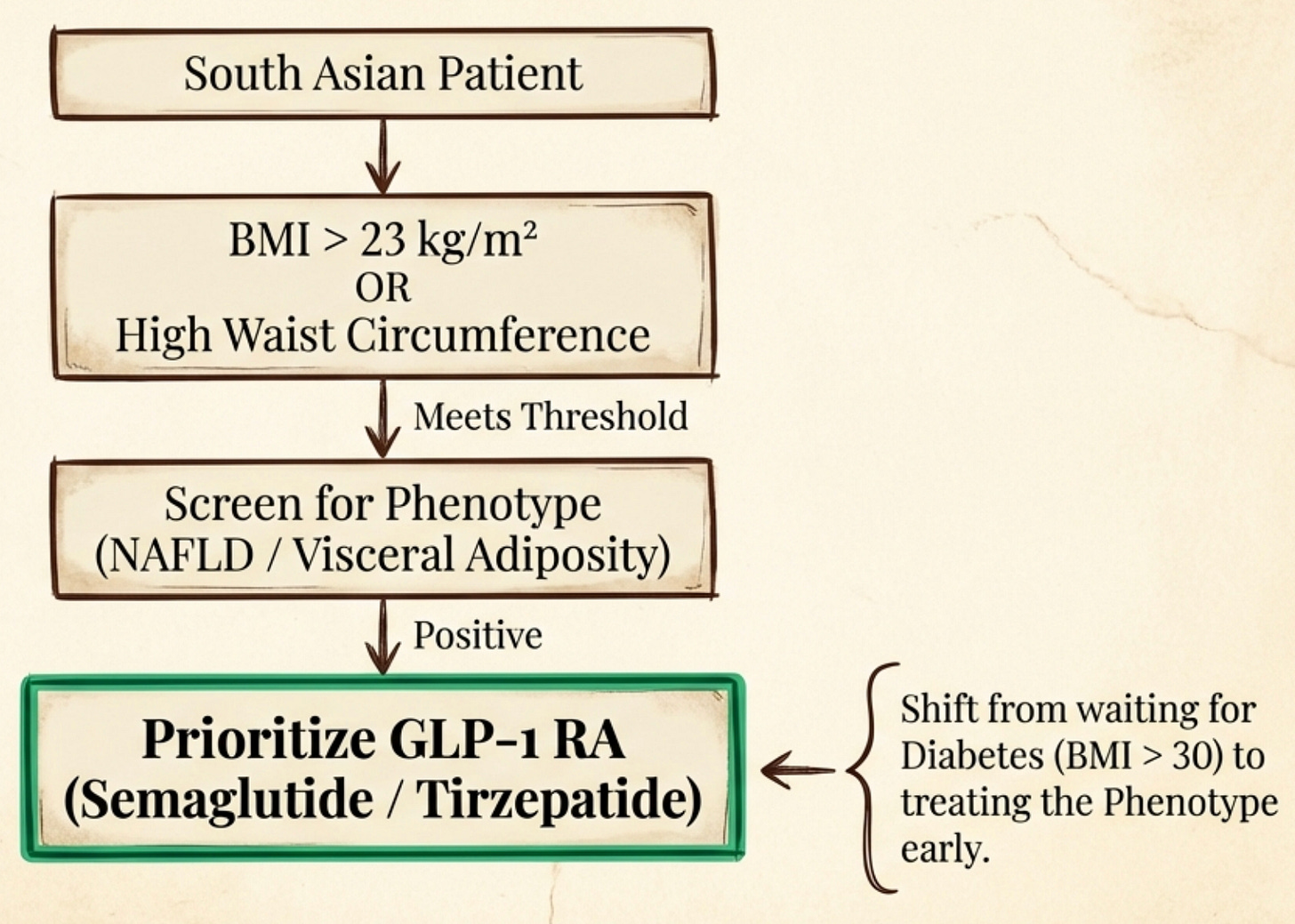
It can be difficult to know when to move from lifestyle-only to medical intervention. Based on the South Asian phenotype specific metrics we have established so far, you might consider asking your doctor about the GLP-1 class earlier if you meet these criteria:
Waist-to-Height Ratio: Is your ratio >0.5 despite a “normal” BMI?
Fasting Insulin: Is it consistently high (>10 uIU/mL), or is your HOMA-IR elevated?
Liver Health: Do you have MRI or Ultrasound evidence of fatty liver, or elevated ALT levels?
HbA1c Trend: Is your A1c drifting up year over year, even if pre-diabetic?
Family History: Is there a strong family history of early T2D or heart disease?
If you check multiple boxes, the metabolic bottleneck may already be present.
Too often, we wait for the crash, the heart attack, the diabetes diagnosis, or the kidney failure, before we act.
At Zinda, we argue for radically proactive metabolic defense, and urge physicians to consider GLP-1s much earlier than they would in other populations. If biomarkers (high insulin, fatty liver, rising HbA1c) show mitochondria are struggling, these tools should be considered now to preserve your organ health, rather than waiting 10 years when the damage is irreversible.
They are not a magic wand, but they are a powerful catalyst.
They work best when placed into the a South Asian focused framework, impeccable nutrition, heavy resistance training, and a deep understanding of your own biology. Why biological first principles matter.
-Omar